Moment that mattered: Trial results show a new drug slows Alzheimer’s disease by a third
In issue 51 we spoke to neuroscientist Professor John Hardy about a medical breakthrough 30 years in the making
3rd May 2023 (Taken from: #51)
In 1992 neuroscientist John Hardy published a paper with an astonishing hypothesis that could change the world: he thought he had found the key to curing Alzheimer’s disease. Alzheimer’s is the most common form of dementia and slowly destroys the memory and thinking skills of those affected. Hardy’s research had identified a specific group of proteins that builds up in the brain of Alzheimer’s sufferers. “When we first found amyloid proteins, we thought that anti-amyloid drugs would be the silver bullet,” he says. “That proved not to be the case.”
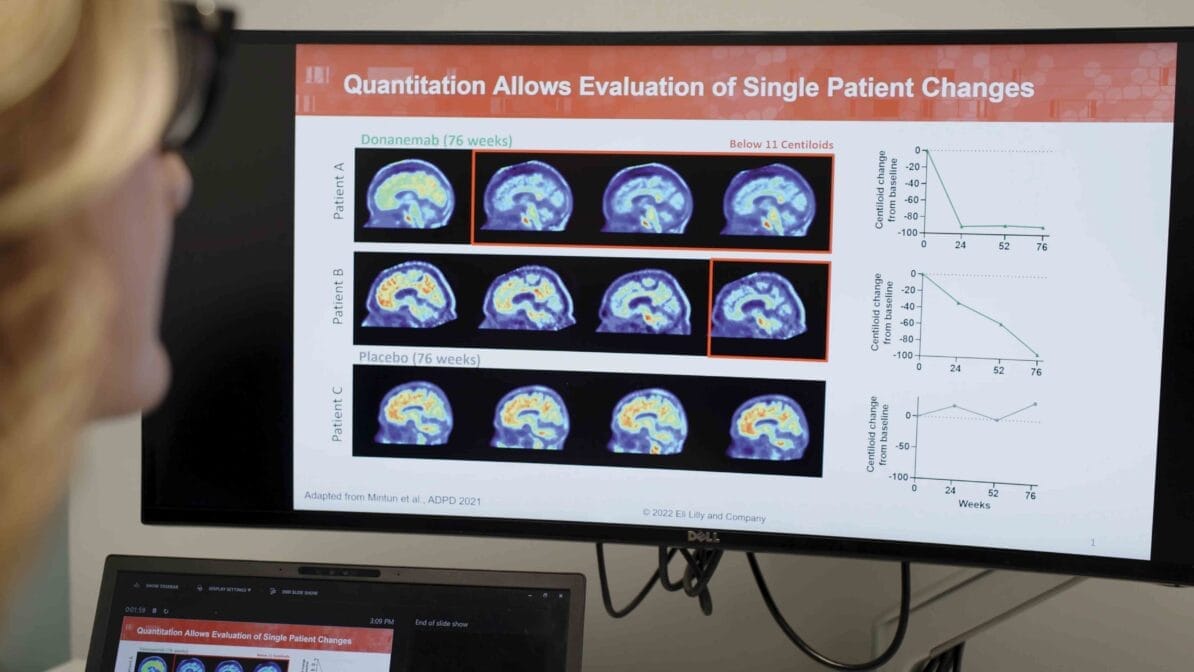
Over 30 years of tests followed, each failing to provide the breakthrough Hardy had hoped for. Then on 3rd May 2023, the results of an antibody therapy study were announced. They showed that a new drug, Donanemab, which targets the amyloid proteins Hardy had identified, had slowed the pace of Alzheimer’s development by a third. “I was really pleased, but also relieved,” says Hardy. “People were telling me that the amyloid hypothesis had been a very expensive and time-wasting red herring, so I was certainly feeling the pressure. It took longer than we would’ve ever thought, but it’s really good to see a payoff.”
The trial of Donanemab, which has been developed by the US pharmaceutical company Eli Lilly, follows news of similar results for Lecanemab – a rival drug from Japanese firm Eisai. In November 2022 it was announced that in trials Lecanemab, which also targets amyloid proteins, had slowed down the speed at which memory and thinking skills got worse by 27 percent. “There are now two drugs which slow the disease by between 25 and 35 percent in the first trials,” says Hardy, who is the chair of Molecular Biology of Neurological Disease at the UCL Institute of Neurology. “This is good news, not only because it slows the disease, but also because it teaches us what we need to do to amyloid [proteins] to be successful. Just as the Wright brothers’ first flight taught people what they needed to do to get a machine off the ground, these trials show others the way.”
Beta amyloid is a sticky gunk that builds up in the spaces between brain cells forming the distinctive plaques in Alzheimer’s sufferers that Hardy helped to first identify over 30 years ago. “The amyloid builds up in the brain and increases tangle formations,” he explains. “The simplest way to describe it is that these tangles sort of strangle the neural cell.”
Just like the Wright brothers’ first flight taught people what they needed to do to get a machine off the ground, this shows others the way”
Donanemab and Lecanemab are both antibodies engineered not only to stop the production of amyloid but to clear any existing build up. “There’s been so many amyloid drugs that have failed over the years, and one of the major reasons is that they stopped amyloid deposition, but they did not remove the amyloid that was already in the brain,” says Hardy. “These two drugs do that.”
While optimistic about the future, Hardy is keen to point out the reality of the trial results. “Clearly, slowing a disease by 25 to 35 percent is good, but it’s not great,” he says. “Let’s say that you’re five years from diagnosis to nursing home care. At the moment, if you were put on the drug, it would suggest you might be six and a half years from diagnosis to nursing home care, so it’s a definite improvement and statistically significant, but it’s not the answer we want in the longer run. One hopeful interpretation, and I emphasise the word hopeful, is that if we got in earlier when there’s less amyloid, we might have a larger effect.”
There are significant risks to consider too. “Very occasionally it can cause a haemorrhage, which, even more occasionally, can be fatal,” says Hardy. “I think it’s worth noting that all drugs have downsides, that’s something people need to be realistic about. Alzheimer’s is a fatal disease, and this is a very serious but rare outcome. In my mind that is the price of it.”
It is not the only price that will be considered if the drugs are to be used in the UK. Early figures suggest that both will cost in the region of £21,000 per patient per year. “On top of that price, you’ve got the price of giving the drug and of the safety monitoring by the NHS,” notes Hardy. “The real price is probably twice the price of the drug”.
In July Lecanemab received full approval by the Food and Drug Administration for use in the US, with a decision on Donanemab expected before the end of the year. It remains to be seen if the authorities in the UK will follow suit. “I think that it’s very likely that the Medicines and Healthcare Products Regulatory Agency will approve it,” says Hardy, who consulted on the development of both drugs. “A far harder fight is going to be with NICE [The National Institute for Health and Care Excellence], the regulatory authority which will ask: ‘Is this drug value for money for the NHS?’. On the one hand, it’s going to slow nursing home care, and on the other, it’s going to cost a lot to administer.”
People with Alzheimer’s disease in their family are desperate for anything to save them in some way”
Hardy believes the two new drugs will advance Alzheimer’s therapies in a similar way to treatments for multiple sclerosis (MS). “The first treatment for MS was called interferon,” he says. “This was quite an expensive drug which had unpleasant side effects and had marginal efficacy. What that did was cause the NHS to get organised so that when better drugs came out – and there’s now a whole series of better MS drugs – the clinicians and the clinical services were organised to properly use them. That’s what we need to do now with Alzheimer’s disease.”
According to Hardy further breakthroughs will follow, not just for Alzheimer’s but for other complex diseases such as Parkinson’s. “I think it’s quite clear that amyloid drugs are part of the answer, but that we need to find other mechanisms to hit other parts of the pathogenesis [the way the disease develops],” he says. “The whole thing has been a learning process, and we now understand things better. I don’t think it’ll take 30 years next time. I hope we can do it in five to ten years.”
For all the promise of the future, on 3rd May Hardy found himself thinking about the past. In the 1980s Carol Jennings was a schoolteacher from Nottinghamshire. Within a short period of time her father and four of her aunts and uncles were diagnosed with Alzheimer’s disease. With her family’s history with the disease, Carol volunteered for a trial, which helped Hardy to develop his ‘amyloid hypothesis’. Following Hardy’s paper, the number of new clinical trials targeting Alzheimer’s disease worldwide increased from just 10 in 1999 to 120 in 2009. There are currently a record 187 clinical trials in the Alzheimer’s drug development pipeline.
Jennings spent 25 years participating in medical research. Throughout the trials, she always refused to test if she had inherited the gene that leads to the specific form of Alzheimer’s her family had suffered from. Sadly in 2012 Jennings was diagnosed with the disease. She was just 58. She is now one of the estimated 46.8 million people living with dementia worldwide, with these numbers expected to double in the next 30 years. Since her diagnosis, she has deteriorated quickly and is now bedbound and in the later stages of the disease.
“It is just one family, and of course there are many others in similar circumstances,” says Hardy. “But Carol was the reason I was feeling emotional when the announcement was made. People with Alzheimer’s disease in their family are desperate for anything to save them in some way. I don’t like comparing diseases, but this is one we have to win.”
People worried about themselves or a loved one being impacted by Alzheimer’s disease can find support and a symptoms checklist at alzheimers.org.uk
Slow Journalism in your inbox, plus infographics, offers and more: sign up for the free DG newsletter. Sign me up
Thanks for signing up.








