Ketamine: the new Prozac?
As notorious club drug ketamine was reclassified in the UK – putting it on a legal par with heroin – in the US it was being touted as a revolutionary treatment for depression. In DG #21, Mike Mariani reported from the frontline of big pharma’s great white hope

Dr Steven Levine. Photo: Robin Resch
30th November 2015 (Taken from: #21)
Charlie, a 34-year-old from Atlanta, Georgia, had been suffering from depression since he was 20 years old. Depression manifests differently both in degree and kind, and over the years Charlie’s has been severe and intractable. He has been on a litany of antidepressants – Prozac, Cymbalta, Zoloft – none of which had a lasting impact on his symptoms. He eventually came around to trying electroconvulsive therapy (ECT) in 2006 at a mental health treatment centre in Atlanta. The therapy – which involves passing electric currents through the brain while under general anaesthetic, in order to set off seizures and change brain chemistry – just left him numb for a few months, and a decade later he still suffers memory problems that he attributes to the experience. He estimates that he’s experienced seven or eight “major episodes” that left him isolated and disengaged from the world, negotiating “constant streams of negative thoughts” and relentless contemplation of suicide. At one point when he was living in Boston in his late twenties, he even sent his dog to live with his parents in Atlanta because he feared the animal would starve after he’d killed himself.
Four years ago, Charlie attended a music festival in New York with a good friend. The friend suggested that they try ketamine, insisting that it would “enhance” the whole experience. It did. Charlie explains that, after the music festival, “for the next three months, I felt on top of the world.” Shortly after the festival, Charlie wrote that doing ketamine was like “months of mindfulness meditation condensed into snortable form.” At one point he was walking back from one of the shows and he passed a girl working at one of the festival booths. She told him he had the most beautiful aura she had seen all day. In the weeks that followed, the high morphed into something more subtle and sustaining. “After that, I was just so incredibly productive,” he says. A software developer, Charlie wrote an app, started taking improv classes, and described those few months as “a very happy time.”
Nothing has changed about ketamine since its heyday as a dissociative hallucinogen passed around clubs”
Charlie is part of a new generation of depression sufferers who are beginning to discover the singular potential of ketamine in fighting the mood disorder. It’s a strange new role for a medicine invented 50 years ago and best known until now as a battlefield anaesthetic, animal tranquiliser and reprobate club drug. Its path to prominence has been slow, but it may now be poised to become a lifeline for sufferers grappling with what writer Andrew Solomon dubbed the “noonday demon”.
Cat Valium 2.0
In 2010, psychiatrist Steven Levine met with a patient who would permanently alter his view of how to treat depression. The patient had come to Levine for a second opinion. She told him that she had “been through the wringer” of depression treatments, each of which had either had no effect or came with unbearable side effects. She confessed to Levine that, after her failures with all the above-board pharmaceuticals, she began experimenting with cough medicine. It worked better than any of the antidepressants she’d been prescribed in the past.
This piqued Levine’s curiosity. One of the common ingredients in different types of cough medicine is dextromethorphan, or DXM, and Levine quickly deduced that this was the drug responsible for relieving his patient’s depression. “What is it about DXM that would account for her response?” he wondered. He began exploring what other drugs out there closely mirrored the way DXM interacts with the body, and whether those drugs also had antidepressant properties. It was then that he stumbled upon ketamine.

Dr Steven Levine. Photo: Robin Resch
“When I read the papers on ketamine, I had to rub my eyes,” he says. This was 2010, when any discussion of ketamine as a treatment for depression was still muted and apprehensive. It was restrained both by the small sample sizes of early experimental trials administering ketamine to patients with treatment-resistant depression and the inescapable connotations of ketamine itself. But certain aspects of these trials were extremely unusual. Typical US drug trials for new antidepressants stipulate that “non-responders” – individuals with a history of not responding to antidepressant drugs – be excluded from the study. In theory this ensures that the objectivity of the experiment is not marred by chronic non-responders, but in practice it’s also a way to boost your chances of getting good results.
The astonishing thing about the ketamine trials was that researchers were including non-responders. “Here is a study including people who have been sick for years and years and have in some cases tried dozens of medications, and they were including them,” says Levine. The early ketamine trials had a kind of indie integrity, rebuffing pharmaceutical industry trends employed to burnish results, and still ending up with something captivating and influential.
Levine explains that participants in these early trials experienced at least a 50 percent reduction in symptoms after a single dose, in some cases even meeting criteria for remission. After speaking with anesthesiologists about the safety of administering the doses being used in the trials (0.5 mg/kg), Levine couldn’t find a good reason not to begin offering intravenous ketamine infusions. This was a prospective treatment that seemed, improbably, low risk and high reward.

Dr Levine’s ketamine tattoo. Photo: Robin Resch
Since those auspicious early trials in the 2000s, ketamine has continued to build momentum as the most promising new treatment for clinical depression. New trials into its efficacy are currently underway at the National Institute of Mental Health (NIMH), Columbia University Medical Centre and the Black Dog Institute in Australia. A 2013 study by psychiatrist James Murrough at Mount Sinai Hospital found that, of the 73 participants, 64 percent of patients who received ketamine experienced a decrease in depression symptoms within 24 hours.
It’s easy to scoff at the new ketamine frontier as a cynical attempt at repurposing for profit a serious street drug with nicknames like “Special K” and “Cat Valium”. After all, nothing has changed about the drug’s potency and chemical composition since its heyday as a dissociative hallucinogen passed around clubs and music festivals, which begs the question of how, exactly, this is any different than Freud recommending cocaine for depression in the 1880s. And the truth is, it’s still too early to declare definitively that ketamine is an effective alternative to traditional antidepressant pills like Prozac and Cymbalta or, as researchers proclaimed in the journal Science in 2012, that it is the “biggest breakthrough in depression research in half a century.” But one thing is certain: the reinvention of ketamine couldn’t have come soon enough for the psychopharmacology industry.
Lost in the big pharma funhouse
Diagnosed mental illness in America is on the rise, and has been for more than a quarter of a century. In the years since the FDA’s approval of Prozac in 1987, the number of Americans who qualify for social security because of mental disorders has increased by 250 percent, while prescriptions for antidepressants have ballooned by 400 percent.
While most psychiatric drugs fall into one of three categories (antidepressants, antipsychotics and anxiolytics), antidepressants are by far the most lucrative and heavily scrutinised. Antidepressants like Prozac, Zoloft and Paxil are called selective serotonin reuptake inhibitors (SSRIs) because of their effect on the brain: they prevent the reabsorption of serotonin by nerve cells, allowing more of the chemical to flow freely in the brain. SSRIs became so popular and lucrative that they effectively shaped how we thought depression worked. Since these drugs were increasing the amount of specific chemicals in the brain (primarily serotonin, but also in some cases norepinephrine), conventional wisdom in psychiatry came to assume that clinical depression was itself caused by a shortage of these chemicals.
And so the chemical imbalance theory of depression was born. This theory was advantageous in two significant ways. First, it destigmatised depression, casting it as a brain disease with the same irrefutable physiological basis as cancer or diabetes. Second, it solidified SSRIs as not merely happy accidents whose way of interacting with the body happened to treat depressive symptoms, but instead as drugs that were developed specifically to fight the pathology of depression.
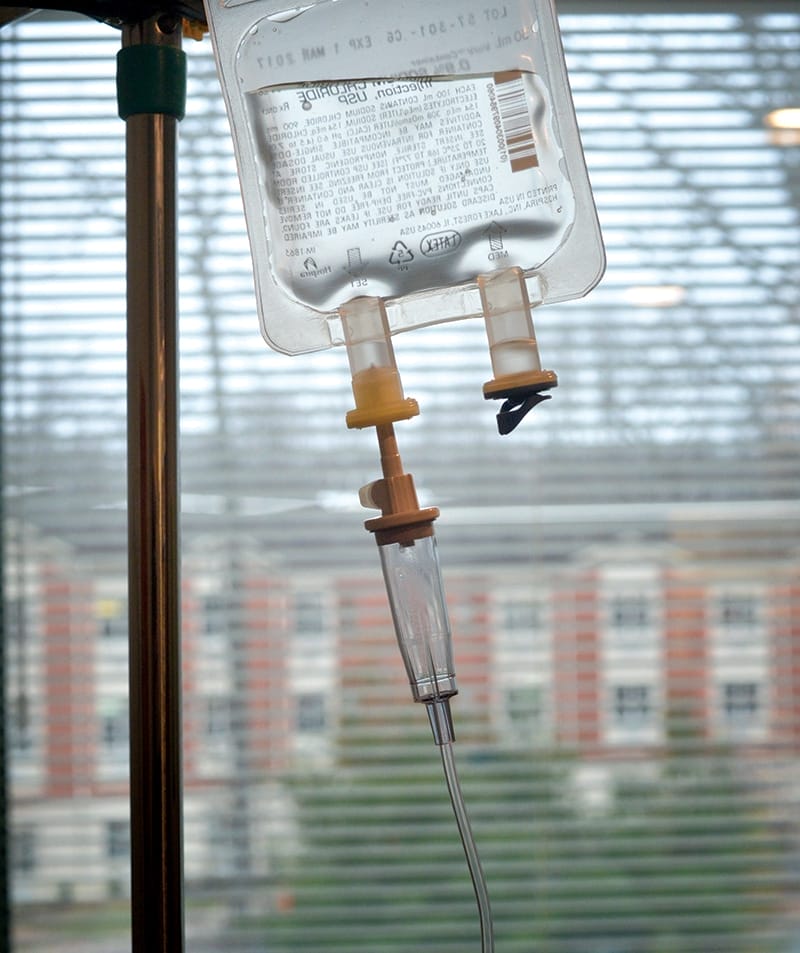
A stand holding a ketamine infusion, used for treating depression. Photo: Robin Resch
Psychiatry was essentially working backwards: instead of identifying the cause of an illness and producing a drug to alleviate it, it identified a drug and produced a cause to justify it. The chemical imbalance theory of depression continues to validate SSRIs and safeguard an antidepressant industry worth around $11 billion a year in the US alone.
Today many psychiatrists have grown disillusioned with the widely popularised notion that depression is caused by a dearth of neurotransmitters like serotonin in the brain. In his 2009 book The Emperor’s New Drugs, Harvard psychologist Irving Kirsch declares that “it now seems beyond question that the traditional account of depression as a chemical imbalance in the brain is simply wrong.” Beyond the discrediting of the chemical imbalance theory, two other factors are becoming damaging to the antidepressant model.
After Prozac went off patent in 2001, drug company Eli Lilly reportedly lost $177 million in a single quarter”
First, antidepressants themselves have not proven to be highly effective in treating depression. A contentious article published in 2010 in the Journal of the American Medical Association even claimed that for most people suffering from depression, placebos were as effective as antidepressants. Some critics have alleged that pharmaceutical company subterfuge can suppress tepid trials like these, publish the successful studies, and whoosh through FDA (US Food & Drug Administration) approval. It only takes a few successful phase 3 clinical trials to receive approval, they say, so pumping enough money into more and more of them can sometimes be enough prove a drug’s viability.
At the consumer level, according to the US National Institute of Mental Health’s STAR*D study, only about a third of patients find any relief from their first antidepressant medication. Many find themselves trying four or five, and some end up on multiple medications simultaneously, forever searching for the Goldilocks zone of happy pills. As Levine told me, “only about half of people are going to respond to SSRIs. If they go through a best practices algorithm of treatments, still only about two-thirds of people will respond.”
In other words, even when patients go through a rigorously tested sequence of treatments (which involves trying one antidepressant for 12 weeks, followed by another, then a combination), a third of depression sufferers still find no relief.
From the perspective of major pharmacology companies like Eli Lilly and Pfizer, the second factor is even more pernicious. US drug patents generally last 20 years. After that, companies lose exclusivity on their drug, as generic manufacturers can begin making much cheaper versions. The “patent cliff,” as it’s known, can cost pharmaceutical companies hundreds of millions of dollars. After Prozac – which had attracted sales of $2.6 billion a year at its height – went off patent in 2001, Eli Lilly reportedly lost $177 million in a single quarter.
Some of Levine’s patients are extremely wealthy, others less so. He recently treated a homeless man who travelled from Texas to see him after hearing about his work”
Just as the market exclusivity afforded to new drugs brings pharmaceutical companies billions, the loss of patents can be financially devastating. Almost all of the major antidepressants, including Zoloft, Paxil, Prozac and Lexapro have gone off patent in the past decade or so and drug companies have lost billions as prized cash cows have been taken to slaughter. They are desperate to fill the financial void left by once-exclusive antidepressants.
For them, ketamine – or at least a variation of it – could be the great white hope of psychopharmacology.
Corporatisation and the kiss of death
When I visit Dr Steven Levine at his Princeton clinic, a suite in a larger medical office building in a remote patch of semi-rural New Jersey, he is arrestingly dapper in a suit and purple tie. His smart dress disguises a secret up his sleeve: he rolls up his shirt to show a tattoo of the chemical formula for ketamine on his forearm.
“I had no intention of going into psychiatry,” he says. “When I went to medical school I went in wanting to be a surgeon. Although I enjoyed surgery I pretty quickly figured out that these were not my people, and a couple of mentors who were psychiatrists seemed to be my people.” Since switching to psychiatry and training at New York Presbyterian and Weill Cornell, he has never looked back. Levine, who is 38, is thin and slightly rangy in a way that is more social than anatomical: his drooping arms and hunched shoulders are a mark of affability, a kind of permanent body language that lets people know that he is accessible, ever-ready to chat, console, explain. His wide-eyed enthusiasm means he never comes across as a pitch man.

A bottle of Prozac. Photo: AP Photo/Darron Cummings
In the consultation room in the back, Levine discusses his clinic’s wide-ranging demographic. The clinic has treated people from the ages of 17 to 88, and patients are equally split between male and female. Some are extremely wealthy, others less so – Levine recently treated a homeless man who travelled all the way from Texas to see him after hearing about his work.
In the next year, Levine hopes to build a foundation arm to his Ketamine Treatment Centres, while also expanding to include centres in Denver, Baltimore and southern Florida. He hopes that the foundation, which he plans to endow by investing a small percentage of each patient’s infusion payment, will allow him to establish a sliding scale of charges based on what patients can afford to pay. Ketamine infusions can cost up to $1,000 (£690), and most patients need a series of the intravenous drip treatments to see longer-term results. Levine even aspires to offer free treatment to those in the direst financial circumstances. The foundation division of Ketamine Treatment Centers also hopes to fund more research into ketamine as a treatment for depression. “Those dollars aren’t coming either from big pharma or the NIMH at this point,” he says.
From a financial perspective, ketamine itself is not particularly attractive to major US pharmaceutical companies. The drug was approved by the FDA almost 50 years ago, back in 1970, and no one is getting a lucrative patent for something that has been available in generic form for decades. As a result, while ketamine is FDA-approved as an anaesthetic, the odds that it will get approval as a depression treatment are nil. This is no bar to Dr Levine’s work – in the US doctors can prescribe FDA-approved medications for unapproved uses and indications, known as “off-label” use. In order to get a drug approved for a specific use, a pharmaceutical company must pour money into enough trials to persuade the FDA of its efficacy. No pharmaceutical company has the financial incentive, however, to put its shoulder into getting a generic like ketamine approved to treat depression.
Since drug manufacturers can’t make any money from ketamine itself, they are instead aggressively pursuing new variants of the drug that will eventually, in all probability, replace it. Hence the irony of the nascent ketamine rage: as the drug gains more widespread acceptance in the medical community, and pharmaceutical companies eye it up as a potential profits bonanza, it is hurtling toward its own obsolescence. It’s being given the big pharma kiss of death.
Typically it’s our dirtier drugs that are more effective, because they have this broader spray pattern of hitting more mechanisms”
Janssen Pharmaceuticals, a division of Johnson & Johnson, is currently working on a variation called esketamine. Rather than being administered intravenously, esketamine will come in the form of a nasal spray. Illinois-based pharmaceutical company Naurex is developing a second ketamine variant called rapastinel. Rapastinel’s upside is attractive enough that Allergan, a global drug manufacturer based in Dublin, Ireland, acquired Naurex for $560 million (£387m) in summer 2015. With his intimate understanding of psychoactive drugs and their chemical effects, Levine cuts through the differences between ketamine and its upcoming variants. “Nasal formulations always have limitations,” he says. Both esketamine and rapastinel are being pushed partly on the basis of their decreased dissociative properties, likely in an effort to distance themselves from ketamine’s reputation as a sketchy hallucinogen. Ketamine, often termed a “dissociative anaesthetic,” produces a sense of detachment from one’s environment and self, inducing a trance-like state. However, says Levine, “being less dissociative isn’t necessarily a good thing. At least for some people the dissociative properties may be part of how this medicine works.”
Levine fears that Janssen and Naurex may narrow the effects of ketamine without fully understanding its multifarious impact on patients. “We get narrower and narrower in our focus of [a drug’s] mechanism, and we wind up watering it down,” he says. “Typically it’s our dirtier drugs that are more effective, because they have this broader spray pattern of hitting more mechanisms.”
Without the “broad spray pattern” that a drug like ketamine affords, patients may not get the same results from the big pharma derivatives. In any case, esketamine, the most well-known of the ketamine variants currently undergoing clinical trials, won’t be publicly available until 2019. And even then, it will probably be very expensive as Johnson & Johnson works to recoup the $300 million it’s spent on research and development.
For now, ketamine has the luxury of not having to compete with the marketing muscle and influence of larger pharmaceutical companies, but it’s unclear how it will coexist with FDA-approved versions in the future.
The battle of the black dog
On 30th November 2015, ketamine was upgraded from a schedule four to a schedule two drug in the UK, meaning that when it comes to medical use it’s on the same level as heroin, morphine and cocaine. Even in its diluted form – patients receive doses about a tenth as strong as those taken by recreational drug users – it’s an extremely powerful drug.
And while a growing number of doctors in the US have a catalogue of success stories from off-label ketamine prescriptions, there are a lot of questions still to be answered about the use of this hallucinogenic tranquiliser for a purpose that has not been officially approved, in the treatment of extremely vulnerable people.
In October 2015, a study was published in the American Journal of Psychiatry analysing 12 of the larger randomised clinical trials on ketamine in recent years. Linda Carpenter is a psychiatrist at Brown and one of the co-authors of the study. “For the very reason that people were starting to get really excited and going into ketamine administration as part of their clinical care, because it was taking off, it was thought that it was really time for the American Psychiatric Association to summarise the state of the evidence and put it in perspective as a guidance document,” she says.
Among the study’s stated conclusions were that “the fleeting nature of ketamine’s therapeutic benefit, coupled with its potential for abuse and neurotoxicity, suggest that its use in the clinical setting warrants caution.” Carpenter explains that one of the largest flaws in current data on ketamine is the lack of longer-term evidence of the drug’s efficacy. “By the time two weeks have passed in most studies, people are back to being depressed again.”
More than anything, this reflects the fact that many of the studies Carpenter and her co-authors looked at only administered one or two ketamine infusions – there were no controlled trials that have looked at longer, repeat dosing protocols. So even if ketamine can be effective in the longer term, and is not just the ephemeral panacea that meta-analyses like this one find it to be, the data simply isn’t there yet. “Where we came down at the end…was thinking a little about both the promise, because ‘wow, ketamine seems to get people better when nothing else has,’ and then all about the limitations,” says Carpenter.
After Charlie’s first euphoric foray into ketamine at a music festival he eventually crashed, which is in keeping with most people’s experiences using the drug as a one-off to fight depression.
Since then, Charlie’s experience receiving the drug in clinical settings has been mixed. He enrolled in a NIMH trial in the summer of 2012 in Bethesda, Maryland, and left crestfallen after the infusion had no discernible effect on his depression. He suggested to the researchers that perhaps he didn’t receive enough of the drug, but because it was a clinical trial, they wouldn’t alter his dosage. Some time later, he contacted Dennis Hartman, whom he met at the NIMH trial and who runs the Ketamine Advocacy Network, looking for another opportunity to try ketamine to fight his profoundly treatment-resistant depression. He found a doctor in Atlanta who was administering ketamine infusions, and in October 2013, he received four infusions over a few weeks.
He now takes a ketamine nasal spray twice a week as maintenance therapy. He says that the mix of infusions and nasal spray “has done a very good job keeping me out of depression.” When I last spoke with him, however, he had recently slipped into a major episode, and had just received the second of six infusions over three weeks; essentially a redux of the acute phase of treatment to beat back the ground depression had gained back. (The most successful clinical trials begin with an acute phase of treatment, where patients are given six infusions over two weeks.)
Ketamine had worked better for Charlie than any of the countless antidepressants he’d tried before, but it was no panacea. Turning a fleeting moment of music festival bliss into something more sustainable has proved dauntingly elusive.
Slow Journalism in your inbox, plus infographics, offers and more: sign up for the free DG newsletter. Sign me up
Thanks for signing up.








